The Connection Between Lower Back and Pelvic Pain In Female: Causes, Science & Relief
Mar 24, 2026
Lower back pain and pelvic pain are both common, and they often show up at the same time. While many people see them as separate issues, new research shows they are linked. The nerves, muscles, and the body’s alarm systems connect these areas. Pain in your lower back can lead to pain in your pelvis, and the other way around. Understanding this link is important for finding lasting relief.
Key Takeaway
You can’t solve pelvic pain without considering your lower back, and you can’t fix back pain without thinking about your pelvis. These areas share nerves and the same alarm system in your body. If one area hurts for a long time, the other often becomes more sensitive too. The best way to heal is to stop focusing only on the painful spot and start calming the whole nervous system that connects both areas.
What are Causes of Lower Back Pain in Females
Figuring out what causes this kind of pain is the first step to feeling better. Pain science shows that the initial tissue or organ cause of pain does not always match how much pain you feel. Two people with the same diagnosis can have different pain levels because the nervous system, immune system and brain has a big impact on how pain is felt and increased. Still, some common causes can set off the alarm system connecting your lower back and pelvis.
Pelvic Floor Dysfunction
The pelvic floor is a group of muscles that forms a hammock across the bottom of your pelvis, supporting your bladder, bowel, and uterus. If these muscles become weak, tight, or out of balance, they cannot do their job well. Research shows that 78% of people with lower back pain also have urinary urgency showing a strong link between pelvic floor problems and back pain. When the pelvic floor is too tight or overactive, it can develop tender points that send pain into the lower back, making it feel like a regular back injury.
Sacroiliac (SI) Joint Dysfunction
The sacroiliac joint links your spine to your pelvis and helps absorb shock as your body moves. If this joint gets stiff, or inflamed, it can cause pain in both your lower back and pelvis. SI joint problems may cause up to 15 to 30% of chronic lower back pain cases. Because of the way the nervous system works, this joint issue can also make nearby nerves more sensitive, so you might feel pain in areas that are not directly injured.
Endometriosis
Endometriosis happens when tissue, called endometrium, which is the lining of the uterus grows outside of it. This tissue can wrap around organs, intestines or irritate pelvic nerves. When these nerves or organs are affected, women can have pelvic pain, GI issues, lower back pain, leg pain, or weakness. Over time, ongoing endometriosis can make the nervous system more sensitive and the brain more protective of that area, so pain can become stronger even when there is no active inflammation.
Hormonal Changes and the Nervous System Hormonal changes during the menstrual cycle, pregnancy, and menopause affect more than just the reproductive organs. In pregnancy, hormones make ligaments looser to prepare for childbirth, which can strain the lower back and pelvis. During menopause lower estrogen levels can affect connective tissue and make the pelvic area more sensitive. Pain science shows that hormones directly affect how sensitive the nervous system is, which explains why many women notice their pain changes during their cycle.
Central Sensitization as a Cause in Itself
For many people with long-term lower back and pelvic pain, the original injury has already healed, but the nervous system, immune system stays on high alert. This is called central sensitization. These systems and the brain start to treat normal body signals as threats, so pain continues even when there is no injury. This pain is real and comes from a sensitive alarm system. Realizing this can help women who have tried treatments without lasting relief.
Symptoms That Show Your Pain Is Connected
Since the lower back and pelvis share nerves, muscles, and the same alarm system, symptoms of connected pain can appear in ways that do not seem related at first. If you notice several of the following signs, it likely means your pain is coming from a system under stress, not just one area.
Pain That Moves or Spreads
You might feel pain in your lower back one day and deep in your pelvis the next. Sometimes, when your back pain gets worse, your pelvic symptoms do too. This shifting and spreading pain is a sign that the nervous system is involved. It happens because the nerves for your lower back and pelvis communicate, so when the alarm system is active, your brain sends pain as a form of learned overprotective patterns. This pattern can be unlearned.
Pain That Does Not Match the Injury
If your scans look normal but your pain feels strong, or if a small movement causes a lot of pain, this is an important sign. It may mean that central sensitization is happening. The pain is real, but the nervous system is making it feel worse by treating normal signals as threats. When pain does not match what doctors see in your tissues, it is a sign that the whole system needs care, not just the body tissue.
Bladder or Bowel Changes
Needing to urinate often, leaking when you cough or sneeze, constipation, or feeling pressure in your pelvis can all happen along with lower back pain. The pelvic floor muscles and the nerves that control the bladder and bowel are connected to the lower spine. When your lower back is stressed, these functions can be affected too.
Pain That Worsens With Stress or Fatigue
If your pain gets worse when you feel anxious, overwhelmed, or tired, this is your nervous system, immune system and brain reacting. Both emotional stress and physical fatigue trigger the same threat response in the brain that causes chronic pain. When your spinal cord is already sensitive, stress makes things worse. This does not mean the pain is 'in your head.' It means your central nervous system (spinal cord and brain) is involved.
Pain During or Around Your Menstrual Cycle
Hormonal fluctuations directly affect how sensitive your nervous system is. Many women notice that their lower back and pelvic pain is worse just before or during their period. This happens because estrogen and progesterone change pain thresholds during the cycle. If your pain follows a hormonal pattern, it is another sign that the connection between your lower back and pelvis is caused by a system-wide response, not just one problem.
A sense of pressure, heaviness, or a feeling that something is 'gripping' deep in your pelvis often occurs along with lower back tension. This means your core muscles are under strain. When your lower back muscles tighten due to pain, the pelvic floor often follows. Many women say this feels like a constant tension they cannot relax, no matter how much they stretch.
The Anatomy of a Partnership: The Core Canister
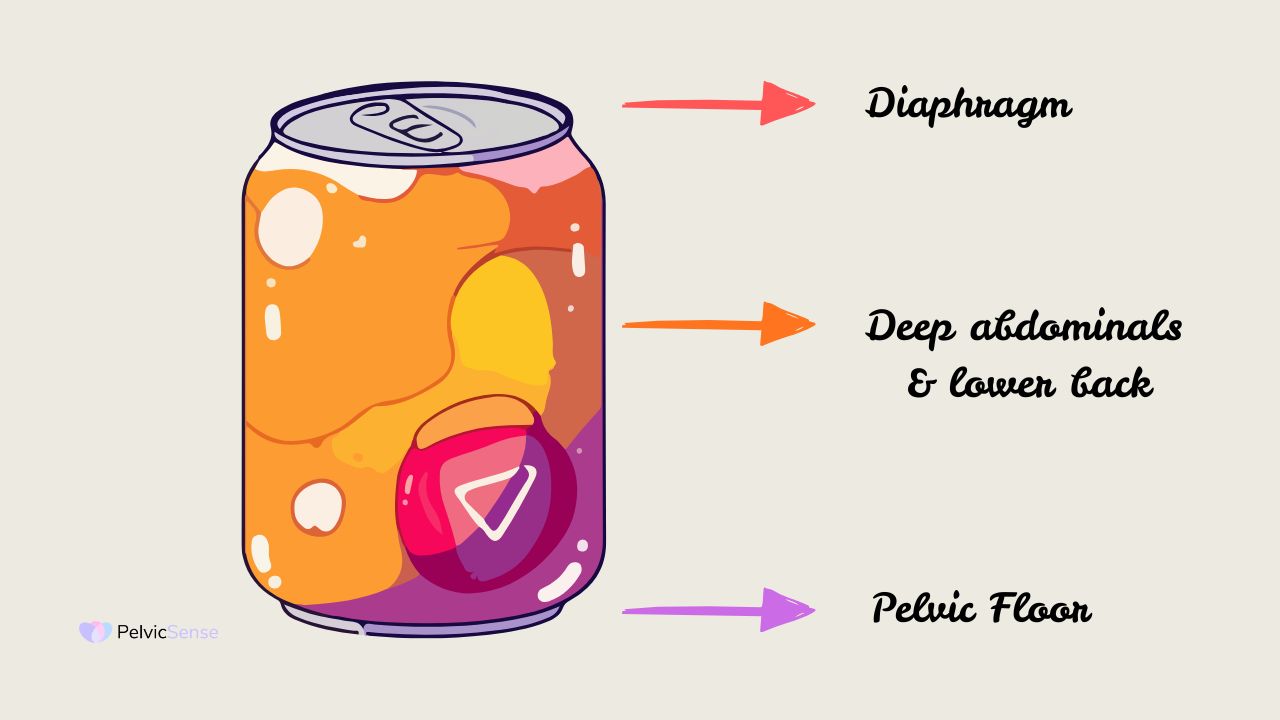
To see why your lower back and pelvis often seem to share pain, it helps to look at how your body is built. Clinicians sometimes call the trunk of the body a pressure canister.
- The Top: The respiratory diaphragm.
- The Bottom: The pelvic floor muscles.
- The Sides: The transverse abdominis and the multifidus (deep back muscles).
These muscles are meant to work together. When you breathe in, your diaphragm moves down and your pelvic floor relaxes a little. When you breathe out, both lift gently. If you have ongoing back pain, your body often tenses up to protect itself, and that tension can make your pelvic floor tight too. In the same way, if your pelvic floor is tight it can pull on your lower back.
If the pelvic floor is too tight, it changes the position of the pelvis and sacrum, pulling on the lower back muscles. This is why many people find their back problems only get better when they also work on their pelvic health, and the same goes the other way around.
Shared Wiring: The Nervous System Connection
The physical link is just part of the story. The way the nerves connect these areas is just as important.
The nerves that go to the skin, muscles, and organs of the pelvis come from the same area in the lower spine, called the lumbar and sacral plexus. Nerves from L1 to S4 control this whole region. When your brain keeps getting danger signals from your lower back, it becomes extra alert. Over time, these signals can spread to nearby nerve pathways.
This is known as referred pain or cross-sensitization. After a while, your brain can’t tell if the problem is coming from your back, bladder, or pelvic muscles. It can feel like the whole area hurts, because your brain is trying to protect you.
The Driver of Chronic Pain: Central Sensitization
When pain lasts longer than the usual three months it takes for tissues to heal, the main cause shifts from the tissues themselves to the central nervous system. The central nervous system consists of your spinal cord and brain, where your spinal neurons, immune cells, and brain neurons communicate. When the spinal neurons receive too many incoming threat messages, the immune system produces more pro-inflammatory molecules, and threat messages bombard the brain. The brain, in turn, becomes overprotective, sending back pain as a signal to you that you are in danger. This process is called Central Sensitization (CS).
When this happens, your nerves and brain stay on high alert all the time, like an alarm that never shuts off. Your body reacts even to small things, and your immune system can join in, making the pain feel worse.
The Role of the "Secret" Immune System
Deep in your spinal cord are special immune cells called glia. For a long time, scientists thought glia just held neurons together. Now we know they act like the guard dogs of the nervous system.
If you’re stressed or have had pain for a long time, these immune cells become more active. They release chemicals that make your nerves even more sensitive. That’s why stress or even changes in the weather can make your pain worse. Your system (spinal, immune and brain) are trying to protect you, but it ends up making the pain last longer.
The Vagus Nerve: The Bridge to Healing

If Central Sensitization acts like the gas pedal for pain, the Vagus Nerve is like the brake pedal.
The vagus nerve is a key part of the parasympathetic nervous system. It runs from the brainstem through the chest and into the abdomen, connecting with every major organ. The vagus nerve also helps control the body’s anti-inflammatory response.
When you activate the vagus nerve, it tells your body to stop staying on high alert. This calms your immune system and your nerves. If you have both back and pelvic pain, calming your vagus nerve is like pressing the brakes on pain. You can’t just stretch or push through the pain. You need to show your central nervous system that you are safe so your brain receives safety messages and the pelvic and lower back muscle can ease, soften, regain full movement and strength.
Mind-Body Practices: Sending "Safety Messages"
At PelvicSense Home Program we help people move from a state of danger to a state of safety. Your brain will only turn off the pain response when it has enough proof that you are safe. We give this proof through teaching you how to send micro moments of safety messages throughout the day, make sleep a priority, shift from thinking and saying natural negative, what if, worry statements to calming, positive statements. The program includes 50 Pelvic Positive Affirmation statements that you can review and choose to use for the next three months.
1. Diaphragmatic Breathing (360 Breathing)
The diaphragm is the top of the core canister and is closely linked to the autonomic nervous system. This makes breathing the fastest way to reach the vagus nerve. When you breathe deeply into your ribs and belly, you move the pelvic floor and lower back muscles, giving them a gentle stretch. This tells your brain, "We are breathing deeply, so we must not be in immediate danger."
2. Pain Neuroscience Education (PNE)
Learning how pain works can actually make it feel less intense. When you understand your pain comes from a sensitive alarm system, not from broken bones or torn muscles, your brain feels less threatened. This helps reduce the pain.
3. Somatic Tracking
Somatic tracking is a gentle mind-body technique that helps you change the way your brain responds to pain. It means paying close attention to the sensations in your body like tightness, tingling, or discomfort without judging or fearing them. You observe the feeling with curiosity, almost like you’re a scientist noticing what’s happening. Instead of thinking, My back is killing me, you might say, “There’s a sensation of tightness in my back, but I am safe right now.
With practice, this helps you break the habit of reacting to pain with fear, tension, or worry. Over time, your brain learns that these sensations are not dangerous, which helps turn down the pain alarm system. Somatic tracking can be paired with calm breathing and gentle movement, making it a powerful tool for retraining your nervous system and promoting real healing.
Why "Calming" Works Better Than "Fixing"
Many treatments focus on stretching, surgery, or medication. These can help at times, but for long-lasting pain, they often don’t work because they only treat the symptoms, not the real cause a sensitive nervous system.
When you focus on calming the nervous system:
- Muscle guarding naturally releases: The brain stops sending the contract and protect signal to the back and pelvic floor.
- Blood flow improves: The fight or flight response (vasoconstriction) ends, allowing fresh blood to nourish the tissues of the spine and pelvis.
- The Neuro-immune system resets: Glial cells return to their resting state, and the neuro-inflammatory soup is cleared away.
A Structured Way to Apply These Techniques
- Start With the Breath, Every Time
- Layer in Education Before Movement
- Use Somatic Tracking During, Not Just After
- End With Rest and Integration
- Build Consistency Over Intensity
Frequently Asked Questions
Why do lower back pain and pelvic pain happen together?
The nerves and muscles in your lower back and pelvis are closely connected. If one area has pain, the other often feels it too because your body’s alarm system can’t always tell the difference between them.
Can stress make my back or pelvic pain worse?
Yes! When you’re stressed, your body’s alarm system becomes more sensitive. This can make back or pelvic pain feel worse, even if there’s no ongoing or new lower back or pelvic tissue damage.
What’s the best way to start calming my pain?
Simple mind-body practices like deep breathing, learning about pain, and noticing your sensations without fear can all help calm your nervous system. These tools help your body feel safe, which helps reduce pain over time.
If stretching and medication haven’t helped, what should I do next?
If traditional treatments haven’t worked, try focusing on calming your whole system. This means teaching your brain and body that you are safe using gentle movement, education, and relaxation. Changing patterns through neuroplasticity needs at least 3 months of practice before noticing significant improvements. Patience and consistent practice is needed, not to look for a quick improvement.
Conclusion
To really heal back and pelvic pain, you need to understand these areas work together. It’s not just about muscles or bones it’s about your whole system. When you focus on calming your body and your brain, you can finally break the pain cycle and get your life back.
If you have been caught in a loop of back and pelvic pain understand that your nervous system has learned a protective pattern. By using mind-body tools such as nervous system regulation, diaphragmatic breathing, and pain education, you are teaching your brain a new way of responding. You are rewiring pain pathways through consistent practice and education.
References
- Dufour, S., et al. (2018). "Association between lumbopelvic pain and pelvic floor muscle function." Journal of Women's Health Physical Therapy.
- Fitzcharles, M.A., et al. (2021). "Nociplastic pain: towards an understanding of prevalent pain conditions." The Lancet.
- Woolf, C.J. (2011). "Central sensitization: Implications for the diagnosis and treatment of pain." Pain.
- Moseley, G.L., & Butler, D.S. (2017). Explain Pain Supercharged.

